Knee osteoarthritis and knee replacements (TKR) are very common. Whilst the vast majority of replacements are completely successful and result in a renewed quality of life, a small minority of patient’s following a TKR have ongoing symptoms and limitations. In addition many patients are keen to avoid a knee replacement for many reasons.
These ongoing symptoms can include :
In some instances these symptoms may be related to the joint itself or other mechanical causes, however in many cases no clear cause can be found.
There is increasing evidence and literature demonstrating an alternative cause of these symptoms may be associated with abnormal blood vessels forming in the tissues surrounding your knee joint. This can occur from osteoarthritis itself or as part of an abnormal healing process following knee surgery, new arteries can grow within and around the joint (known as the synovium). This is called “synovial neo-revascularization” (NSR).
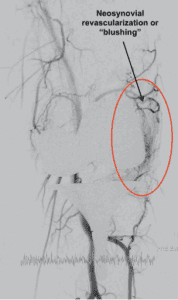
Figure 1 : Angiographic evidence of NSR
These new blood vessels can result in :
The treatment of NSR has been shown to improve outcomes in primary arthritic knees and following TKR.
Your Orthopaedic Surgeon would have excluded all alternate causes of pain following your knee replacement and when no other causes can be found, they may refer you to Mr Ponosh to investigate and treat alternate causes such as synovial neo-revascularization.
In many cases, your surgeon may refer you to Mr Ponosh to see if the treatment of NSR may postpone or delay the need for a replacement or improve your symptoms.
Mr Ponosh may organize a number of investigations to exclude other possible causes of pain and discomfort. These tests are bulk billed and conducted in Mr Ponosh’s rooms. They may including :
There is currently no definitive non-invasive test however available to diagnose NSR.
Conservative
In some cases even though NSR is thought to be present, Mr Ponosh and your Orthopaedic Surgeon may decide a conservative approach is best suited to you. This decision is always made after a thorough discussion with you and the reasons explained. Of course, you can always choose a conservative treatment course which may include pain killers and physiotherapy.
Geniculate Embolization
Whilst the NSR and its treatment is gaining increasing acceptance and a strong body of international evidence supporting its effectiveness and safety in post TKR chronic symptoms, it is still considered a novel and relatively new procedure. It is not widely undertaken however, the elements of the procedure are routine and well accepted vascular interventions.
The treatment for NSR is through a procedure known as a Geniculate Artery Embolization (GAE). The abnormal vessels that cause NSR arise from vessels which supply the knee and surrounding tissues known as geniculate arteries. Geniculate arteries are very small branch arteries that arise from the main arteries of your leg around your knee. GAE is a minimally invasive angiographic procedure to identify these abnormal vessels and embolize (block them). This stops inflammation, leaking and bleeding associated with NSR and hopefully reduces or resolves your symptoms.
The procedure although novel, is extremely low risk and safe. Whilst no guarantee of outcome can be made, often patients referred for consideration of GAE have exhausted all other management options and have ongoing significant disability and lifestyle impairment effective their day to day lives. In this situation, given the low risk procedure and documented successful outcomes, GAE is a worthwhile and appropriate intervention.

Figure 2 : Resolution of NSR following Embolization
The procedure :
This is because :
Risks of GAE
Bleeding
As the operation is performed on blood vessels a small amount of bleeding can sometimes occurs. This is often easily treated with some pressure but it is common to have some bruising to the area after the procedure. You may also develop a small lump which will resolve by itself. Serious bleeding is very uncommon but may require an additional procedure to correct.
False aneurysm
Very rarely a lump may occur which is in flow with the artery. This is because of some continued bleeding from the puncture site. This is called a pseudoaneurysm. This pseudoaneurysm may settle by themselves whilst other may require an additional procedure to fix them.
Pain/Discomfort
Pain and discomfort is usually minimal during the procedure and after. Occasionally you can get some bruising and discomfort to the groin in the following days but this is minor. If you are concerned or the pain is significant please seek advise.
Allergic reactions to the dye
Very rare
Damage to blood vessels
Usually these problems can be dealt with at the time of the procedure, but in rare instances, repair is necessary.
Equipment failure
It is theoretically possible for a catheter, wire or device to break and leave a fragment inside the body. This is extremely rare.
Failure of technique
Occasionally it is not possible to perform the procedure does not show the desired result. In very rare circumstances a failed procedure can actually make the blood flow worse. Catastrophic outcomes are very rare.
Kidney damage
The dye used is excreted via the kidneys, which in most patients is completely normal. However, especially in patients poor kidney function, the dye can lead to deterioration in kidney function. Angiograms are used in patients with kidney disease often and safely but additional precautions are required such as admission the night before the procedure, additional fluids and modifying your medications. Mr Ponosh will discuss these with you. Patients on dialysis do not need additional precautions and angiograms are completely safe.
3. Standard risks of general anaesthetic and regional anaesthesia
Your risk for anaesthetic will be assessed initially by Mr Ponosh, but definitively by his Specialist Anaesthetists. They will discuss the low risk in detail.
Pain post procedurally is normally minimal, managed with simple pain killers